“Employees want to know why they have to produce and deliver services by using certain methods. To be good at holding your staff accountable, you must be good at teaching. Teach about the consequences.” — Crucial Accountability
Did you know that poor documentation quality has a bigger financial impact than productivity does? It’s true! In general, while you save $0.02 for every 1 percent productivity increase, billing minutes pulled out during an audit will have a much greater financial loss:
RUC x 14 days (647.94/day = $9,071.16)
RVC x 14 days ($555.85/day = $7,781.90)
In conclusion, one billing minute removed due to unskilled documentation could result in a $1,289.26 loss.
DOR Role
What is the role of the DOR? We define it as follows:
- Commit to auditing documentation
- Set expectations at the interview
- Give positive feedback as often as constructive feedback
- Audit evaluations and MD orders to catch errors and monitor trends
- Initiate a “standardized test” day
- Include standardized test in “precautions” on POCs, to ensure staff re-test
- Monitor progress notes to look for trends
UR prep and care plans must:
- Create effective care plan process
- Frequently attend care plans to review weekly documentation
- Prep for UR using the “weekly status report”
- Ensure therapists are testing goal-related areas and that discharge dates are
- appropriate
- Report standardized test scores/ADL score during UR
Teach the Why
In order to hold staff accountable for skilled documentation, it’s important to engage your team in dynamic thinking about the “why” behind what they do. That is, educate them as to why quality documentation is important, as it not only reflects their clinical skill, but also ensures we can be billed for services and therefore has a financial impact. Finally, provide lists of commonly used skilled terms descriptive of therapists’ actions.
MSCA Data
Skilled documentation is a critical part of our systems at Granite Creek Health and Rehabilitation. By implementing training in this area, we saw an improvement in the MSCA therapy score and a decrease in the financial error rate:
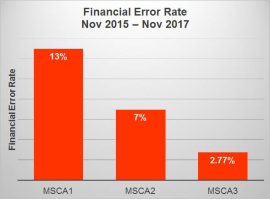
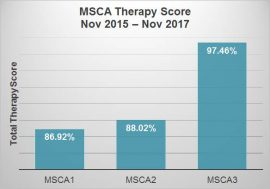
By Larissa Osio, DOR, MS OTR/L, Granite Creek Health and Rehabilitation, Prescott, AZ
View full poster here: Accountability and Skilled Documentation -Granite Creek


 Clients with dementia living in skilled nursing facilities have occupational needs that are often unmet. Individualized care approaches and engagement in meaningful activities are effective non-pharmacologic approaches to dementia care. However, they are infrequently implemented in SNFs, and patients with dementia are often medicated with antipsychotic medications to manage behavioral symptoms related to dementia.
Clients with dementia living in skilled nursing facilities have occupational needs that are often unmet. Individualized care approaches and engagement in meaningful activities are effective non-pharmacologic approaches to dementia care. However, they are infrequently implemented in SNFs, and patients with dementia are often medicated with antipsychotic medications to manage behavioral symptoms related to dementia.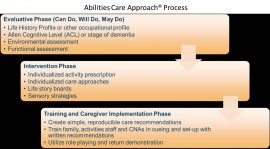

 After noticing a recent increase in falls and fall-related injuries at our building, we wanted to better understand the mechanisms of the falls and implement a comprehensive, interdisciplinary fall prevention program.
After noticing a recent increase in falls and fall-related injuries at our building, we wanted to better understand the mechanisms of the falls and implement a comprehensive, interdisciplinary fall prevention program.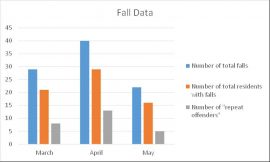

 At Grand Terrace Rehabilitation and Nursing, we have implemented an Oral Hygiene Program with great success for residents. The purpose of the program is multifold:
At Grand Terrace Rehabilitation and Nursing, we have implemented an Oral Hygiene Program with great success for residents. The purpose of the program is multifold:
 As healthcare professionals, we often discuss dementia in the context of various stages, that is, how far a person’s dementia has progressed. Sometimes, we’ll define a person’s stage simply as early-stage, middle-stage or late-stage; however, to be more exact, we use the Global Deterioration Scale (GDS), which assigns seven different dementia stages based on the degree of cognitive decline.
As healthcare professionals, we often discuss dementia in the context of various stages, that is, how far a person’s dementia has progressed. Sometimes, we’ll define a person’s stage simply as early-stage, middle-stage or late-stage; however, to be more exact, we use the Global Deterioration Scale (GDS), which assigns seven different dementia stages based on the degree of cognitive decline. Our skilled population has gradually shifted from traditional Medicare Part A to Managed Care Part A. Therefore, our treatment focus has had to shift as well. We are no longer focusing on progressing to prior level of function, but rather progressing to next level of care.
Our skilled population has gradually shifted from traditional Medicare Part A to Managed Care Part A. Therefore, our treatment focus has had to shift as well. We are no longer focusing on progressing to prior level of function, but rather progressing to next level of care. Last year, Ensign therapists were introduced to a new balance pad system called the Sanddune Stepper. It is said to have significant effects on improving proprioception and ankle strategy in patients with a neurological diagnosis.
Last year, Ensign therapists were introduced to a new balance pad system called the Sanddune Stepper. It is said to have significant effects on improving proprioception and ankle strategy in patients with a neurological diagnosis.