By Elyse Matson, MA CCC-SLP, Clinical Resource
Cognition and Swallowing are among the common challenges persisting for many Americans after COVID-19. Speech-Language Pathologists (SLPs) can help patients regain health and quality of life.
With an estimated 10 to 30% of COVID-19 survivors experiencing a post-COVID-19 syndrome, including brain fog and swallowing difficulties, it is more important than ever to utilize the full range of services provided by SLPs.
The pandemic tested everyone as a society, but one of the persistent challenges is the daunting set of difficulties many of our residents and those in our communities are experiencing after contracting and recovering from COVID-19. Many continue to demonstrate diminished function, including with cognitive skills, communication of needs and swallowing abilities.
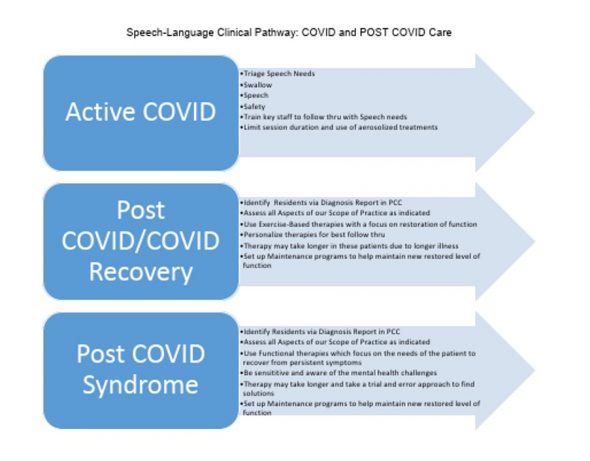
This is an excerpt from the new COVID-19 Clinical Pathway, available on the Portal. This tool guides SLPs through the specific treatment needs of residents at various phases of recovery from COVID-19.
Impairments SLPs can assess
● Cognition
Many residents who had COVID-19 report persistent brain fog as a debilitating symptom after recovering from the virus. This can prevent a return to home as well as impact independence with ADLs. SLPs engage with individuals to improve their memory, attention, organization and planning, problem solving, learning and social communication — such as re-learning conversational rules or understanding the intent behind a message or behind nonverbal cues. The focus is on the person’s specific challenges as well as regaining the skills that are most important to their daily life and priorities.
● Swallowing
Residents diagnosed with COVID-19 may experience swallowing problems that can put them at risk for choking, aspirating, decreased appetite and diminished sensory feedback while eating (loss of taste and smell). This may be the result of time spent on a ventilator, or it may be another side effect of the virus. SLPs are part of the team who decide on the best course of action with the patient and their family. SLPs may recommend modified textures of food and drink for patients; therapy exercises to strengthen the tongue, lips, and muscles in the mouth and throat; and strategies to make eating and drinking safer, such as modifying the pace of chewing/eating, size of food, and more.
● Communication
People diagnosed with COVID-19 are also experiencing speech and language difficulties. Some, such as those who spent a significant amount of time on a ventilator or experienced low oxygen to the brain, may have muscle weakness or reduced coordination in the muscles of the face, lips, tongue, and throat — making it difficult to talk. Others, particularly those who experienced a COVID-related stroke, may experience aphasia, which makes it hard for someone to understand, speak, read or write. SLPs intervene with patients through targeted therapy to improve their communication and understanding.
People who have severe speech and/or language difficulties may need to find other ways to answer questions or tell people what they want, such as through gesturing with their hands, pointing to letters or pictures on a paper or board, or using a computer. These are all forms of augmentative and alternative communication (AAC). SLPs help find the appropriate AAC method to meet an individual’s needs.
For questions about SLP scope of practice or program development, contact Elyse Matson, SLP Resource, at ematson@ensignservices.net.